Chronic Pain
Personalized medical care for chronic pain, focused on safety, balance, and long-term stability.

Chronic Pain
Personalized medical care for chronic pain, focused on safety, balance, and long-term stability.
Breaking the Cycle of High-Dose Opioid Treatment
Many patients with chronic pain find themselves on high-dose opioid or narcotic treatment plans for months or even years. Most often, this occurs with patients who have suffered a serious injury or accident that caused severe, ongoing pain. Patients who have received high doses of pain medications for extended periods of time may find themselves unable to effectively taper off their medications.
Treatment Tolerance
While opioid medications successfully treat acute pain, they are not effective in treating chronic pain. Following an extended course of high-dose opioids, the brain’s reward system grows accustomed to the regular dose, and requires higher amounts of opioids to achieve only partial relief. This process is called tolerance. This decrease in the potency of the brain’s response can cause additional symptoms, which then exacerbate the original, underlying pain condition. Once the brain has developed tolerance to opioids, it can experience withdrawal when an effective opioid level is not met. Withdrawal symptoms include insomnia, restless legs, irritability, and increased pain in the original site of injury as well as elsewhere in the body.
Chronic opioid use also causes an uncomfortable condition called hyperesthesia — the brain becomes hypersensitive to pain signals from anywhere in the body that would usually be considered mild or unimportant. A patient with hyperesthesia will feel unusual, exaggerated pain when they decrease opioid medications; they will then communicate a higher pain level to their physician, and this will often lead to a diagnosis of chronic pain, sometimes without a detectable physical cause. Subsequent increases in opioid medications to deal with the pain will cause the brain to develop a higher tolerance, which causes increased hyperesthesia and withdrawal symptoms. This leads to an increase in dosage and an ineffective treatment cycle begins.
This cycle is caused by the brain’s increasing tolerance to opioid medications, and way to break the cycle is by switching to a medication that will stop the increasing tolerance in its tracks.

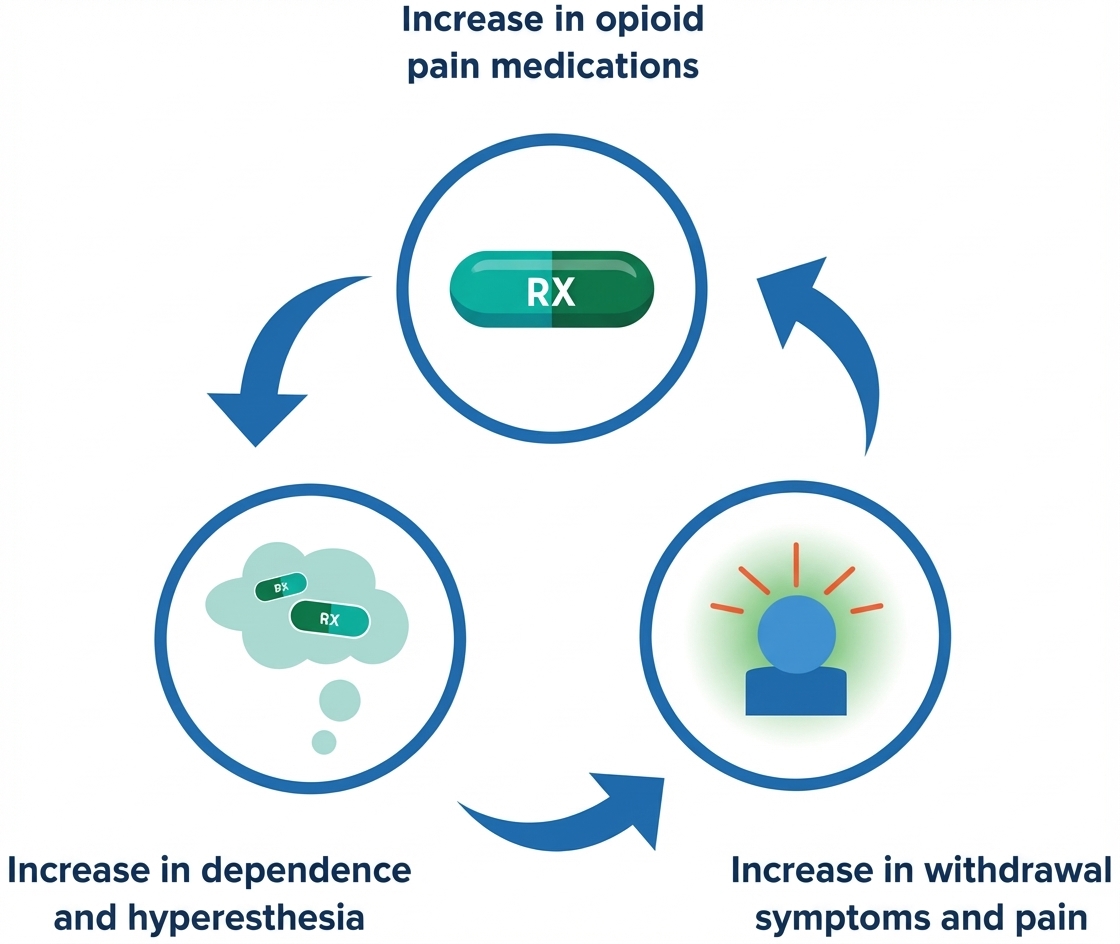
Getting Treatment Back on Track
We can effectively help chronic pain patients to transition to less damaging medications, including buprenorphine, which does not worsen tolerance due to its weak opioid activation. Our procedure was developed by opioid management experts and is carried out in a private, healing atmosphere, where high-quality care, understanding, and compassion lead to long-term success.
After undergoing an effective medication transition, many patients experience significantly improved function, decreased anxiety and depression, improved sleep and energy levels, and most importantly, decreased pain. Patients often discover that what they had assumed to be pain from an injury was actually withdrawal or hyperesthesia, and after medication transition, they no longer need opioid pain medications. Many who continue to have an underlying pain condition find that they can adequately manage their ongoing symptoms with non-addictive options, and even those who still require narcotics often find they require markedly lower doses than previously.

